By Shingirai Vambe
Countries across the globe have been shaken into recalibration, shifting policies and reworking strategies following the return of United States President Donald Trump to the centre of global influence and his renewed stance on cutting financial support to developing and economically struggling nations. Across Africa and beyond, the effects have been immediate and unsettling, particularly for countries that have long relied on donor-funded programmes to sustain critical sectors of their economies.
Zimbabwe has not been spared from the fallout. In the wake of reduced external funding, several non-governmental organisations have been forced to close operations altogether, while others have suspended or scaled down their activities. The ripple effects have been felt across multiple sectors, with the health sector emerging as one of the hardest hit. For years, donor funding had underpinned key health services, particularly those addressing chronic and incurable diseases, rural health outreach, and the welfare of frontline health workers.
The abrupt withdrawal of funding placed thousands of vulnerable citizens at risk, threatening access to life-saving services and exposing long-standing structural weaknesses within the healthcare system. Rural communities were especially affected, as many clinics and health programmes depended heavily on NGO support to function. Health workers in these areas, who had for decades raised concerns over poor conditions of service, inadequate remuneration, and neglect, suddenly found themselves in an even more precarious position.
Against this challenging backdrop, the Government of Zimbabwe has moved to reposition itself as the primary guarantor of healthcare delivery, bringing renewed hope to citizens and health practitioners alike. Central to this shift has been a deliberate policy focus on addressing the long-running welfare concerns of health workers, issues that, for time immemorial, had contributed to low morale, frequent industrial action, and staff migration.
The government, working with the Health Service Commission (HSC), has taken decisive steps to close gaps created by the exit of NGOs. One of the most significant interventions has been the absorption of health professionals who were previously employed under donor-funded programmes into permanent government service. This move has not only stabilised service delivery but has also provided job security and improved conditions of service for thousands of healthcare workers.
Speaking to The Post On Sunday, Health Service Commission Secretary Dr Christopher Pasi said recent developments within the sector point to a marked improvement in labour relations and workforce stability.
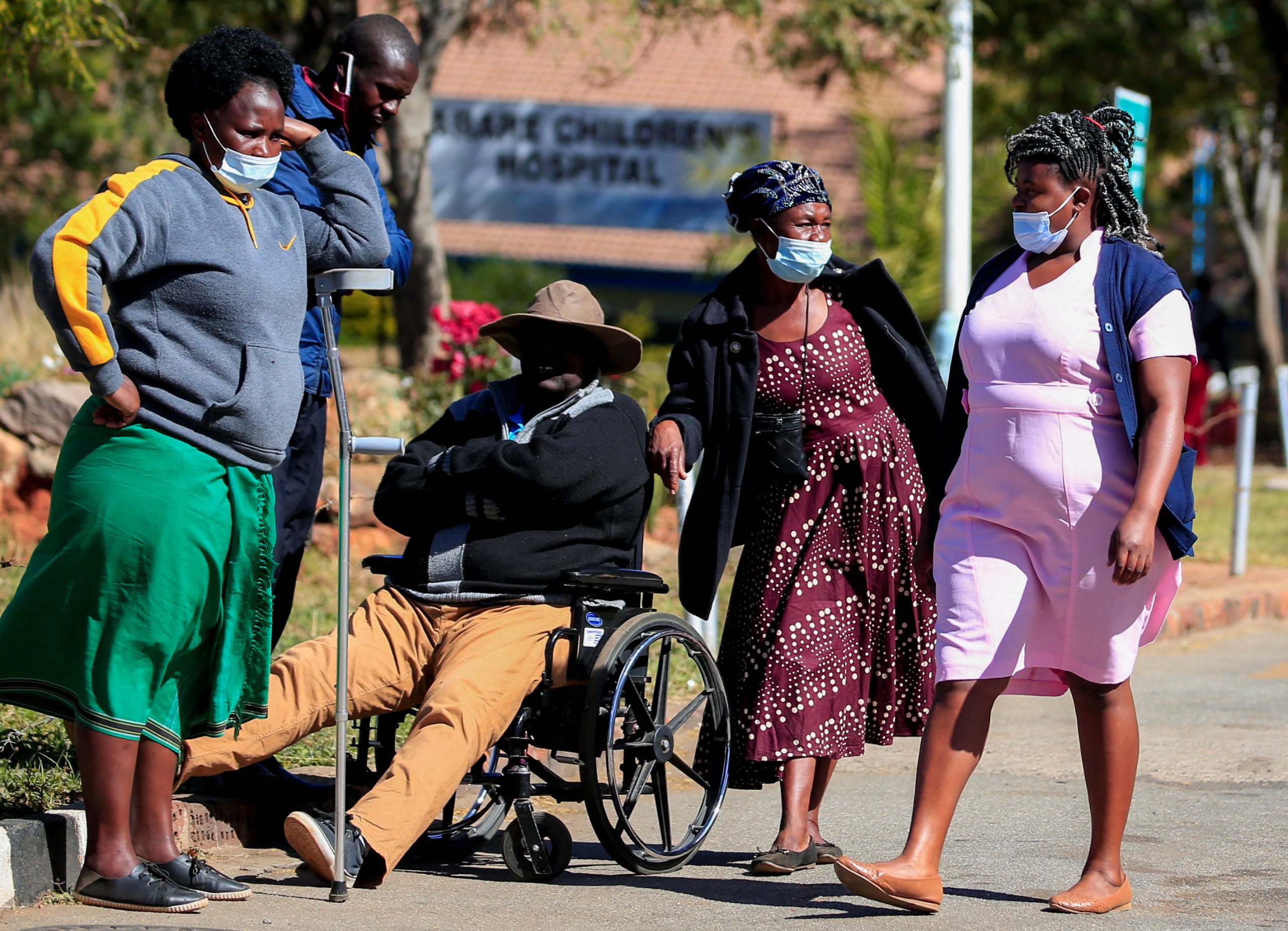
“A noticeable decline in industrial actions, reduced incidence of picketing signals and low absenteeism indicates a more harmonious relationship between health workers and management,” Dr Pasi said.
“This suggests that healthcare practitioners are not only committed to their work but are also feeling more motivated and supported.”
He noted that improved remuneration has played a critical role in restoring confidence within the sector.
“Improved salaries ease financial pressure, helping health practitioners focus more on patient care rather than personal survival. This reduces burnout and improves overall well-being,” he said.
In addition to salary improvements, Dr Pasi highlighted the impact of the Presidential Bonus paid in December 2025, describing it as a direct morale booster.
“As a result of this development, health workers felt appreciated and were motivated to continue delivering quality care,” he said.
Between 2023 and 2025, the Health Service Commission recruited a total of 12,347 health workers, a process guided by staffing needs identified through the Zimbabwe Health Labour Market Analysis conducted in 2022, as well as other staffing requirement indicators. Dr Pasi explained that recruitment efforts are also shaped by the availability of qualified candidates in the labour market.
“Over the years, significant shortages have been observed among specialist cadres,” he said. “While recruitment has improved capacity, these gains have been affected by attrition in certain staff categories.”
To address this challenge, the commission has implemented targeted retention schemes aimed at keeping critical skills within the public health system.
Meanwhile, the Ministry of Health and Child Care (MoHCC) has also seen a notable expansion in its workforce establishment. Currently, the ministry has a total health workforce of 52,874. Of these, 3,119 positions were filled during a rapid staff recruitment exercise conducted by the Health Service Commission in the last quarter of 2025.
The MoHCC staff establishment increased from 51,778 to 57,062 following the creation of an additional 5,284 posts in 2025. Authorities say the remaining vacant posts will be progressively filled to improve the availability, equity, and distribution of health workers across the country, particularly in underserved rural areas.
Efforts to get a comment from the Ministry of Health and Child Care were futile.
Further relief has come through welfare-focused incentives. To date, approximately 7,404 health service members, representing about 14 percent of the workforce, have benefited from the Duty-Free Rebate Scheme, easing the cost of personal transport and improving mobility, especially for those deployed in remote areas.
As external funding uncertainties continue to reshape Africa’s development landscape, Zimbabwe’s renewed emphasis on state-led healthcare financing and workforce stabilisation signals a strategic shift away from donor dependency. While challenges remain, the recent interventions point to a healthcare system striving to adapt, rebuild confidence, and place the welfare of both patients and practitioners at the centre of national priorities.










More Stories
Rural Connectivity Expands Under Zimbabwe’s Broadband Push
IPEC Takes Over NSSA Oversight in Major Pension Shake-Up
Degrees Packed, Dreams Exported